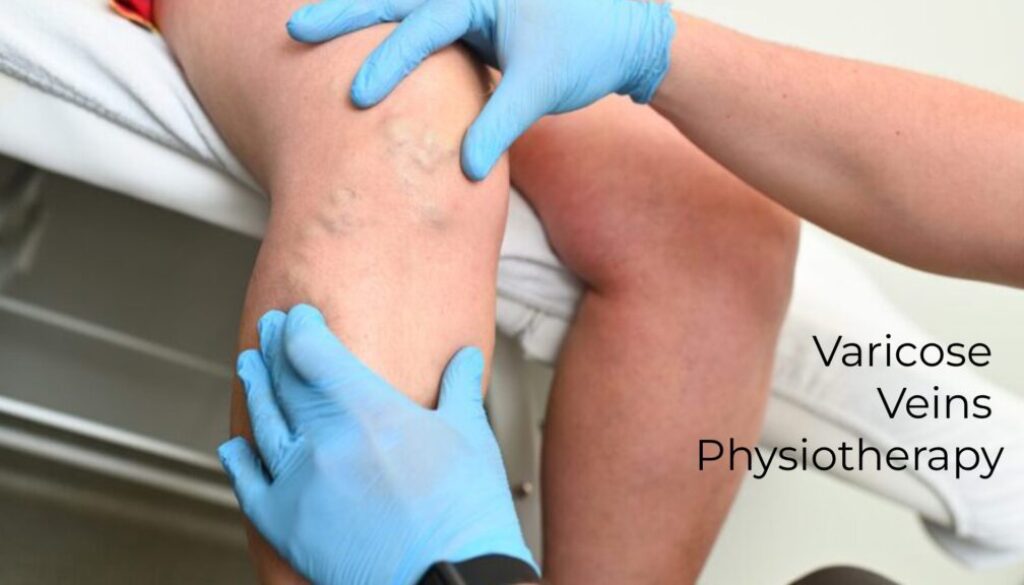
Varicose Veins Physiotherapy: Treatment, Exercises & Recovery Guide
If you have ever noticed swollen, rope-like veins running along your calves or thighs, you already know how uncomfortable varicose veins can be. Beyond the cosmetic concern, they often bring aching, heaviness, cramping, and swelling that make standing or walking a genuine challenge. The encouraging news is that physiotherapy offers a science-backed, non-invasive path to relief — and in many cases, a structured physiotherapy program can delay or even eliminate the need for surgery altogether.
This guide covers everything you need to know: what causes varicose veins, how physiotherapy addresses the condition, which specific exercises work best, what a post-surgical recovery looks like, and how you can access expert care without leaving your home in Bangalore.
What Are Varicose Veins? Understanding the Condition First
Varicose veins are enlarged, tortuous veins that develop when the one-way valves inside your leg veins weaken or fail. Normally, these valves push blood upward toward the heart against gravity. When they malfunction, blood pools in the vein, causing it to stretch, bulge, and become visible beneath the skin.
Medically, the condition is often classified under chronic venous insufficiency (CVI) — a broader term that includes everything from mild swelling to severe venous ulcers. The prevalence of varicose veins in the adult population is estimated at 5 to 30%, and women are more commonly affected than men, particularly after pregnancy.
Common Risk Factors
Several factors increase the likelihood of developing varicose veins:
- Prolonged standing or sitting — a major occupational hazard for teachers, nurses, IT professionals, and retail workers
- Obesity — excess body weight puts greater pressure on the venous valves
- Pregnancy — hormonal changes and increased pelvic pressure compress the leg veins
- Family history — genetics plays a significant role in valve integrity
- Age — vein walls naturally lose elasticity over time, especially after 40
- Wearing tight clothing or habitually using high-heeled footwear
Recognising the Symptoms
The earliest sign is usually a feeling of heaviness or fatigue in the legs, especially at the end of a long day. As the condition progresses, symptoms can include:
- Visible, bulging veins that are dark purple or blue in color
- Persistent aching, throbbing, or cramping in the legs
- Swelling (edema) around the ankles and lower legs that worsens with prolonged standing
- Itching or a burning sensation around the affected vein
- Skin discoloration or hardening (lipodermatosclerosis) in advanced cases
- In severe cases, venous ulcers that are slow to heal
Left untreated, varicose veins tend to worsen progressively and can lead to post-phlebitic syndrome, superficial venous thrombosis, and non-healing leg wounds. This makes early, consistent intervention important.
Why Physiotherapy Is a First-Line Approach for Varicose Veins
Physiotherapy is recommended as a primary treatment strategy for varicose veins across major clinical guidelines because it addresses the root problem: poor venous return and a failing calf muscle pump.
The calf muscles act as the body’s peripheral heart, contracting during movement to squeeze blood upward through the veins. When chronic venous insufficiency sets in, the ankle joint often becomes stiff due to fibrotic tissue buildup, which prevents the calf pump from working correctly. Physiotherapy directly targets this dysfunction by restoring joint mobility, strengthening the calf musculature, and improving overall circulation through a structured rehabilitation program.
A landmark controlled study published in a peer-reviewed journal found that patients who underwent a 24-week combined physical therapy program — consisting of supervised exercise twice weekly plus daily independent sessions — saw venous capacity decrease by an average of 16%, while venous refilling time improved significantly. The control group showed virtually no change. Patients in the treatment group also reported substantially better quality of life scores. These findings confirm that physical therapy offers long-term therapeutic value, not just temporary symptom relief.
Physiotherapy Treatment Approaches for Varicose Veins
A qualified physiotherapist designs a treatment plan based on a thorough assessment that includes the severity of venous disease, ankle range of motion, calf muscle strength, skin condition, and any coexisting conditions. The core physiotherapy interventions include the following.
1. Structured Exercise Therapy
Exercise is the cornerstone of physiotherapy for varicose veins. A well-designed program rehabilitates the calf muscle pump, the primary mechanism responsible for pushing venous blood back toward the heart.
A research study published in the Medical Journal of Dr. D.Y. Patil Vidyapeeth documented a 2-month physiotherapy rehabilitation protocol for a patient with severe varicose veins. By the end of the program, the enlarged veins had reduced in size, discoloration had improved, and associated knee pain had resolved — results achieved purely through physiotherapy intervention with no additional surgery.
The exercises most commonly prescribed include:
Ankle Pumps and Rotations: The patient flexes the foot up and down rhythmically, then circles the ankle in both directions. The protocol by Shah and Sadhu (2022) recommended approximately 810 ankle-toe repetitions per day — a number derived from research showing that 720 repetitions are needed to prevent venous stasis. This exercise is effective because it activates the calf pump without placing significant load on the veins.
Calf Raises: Standing with feet hip-width apart, the patient rises onto the toes and slowly lowers back down. This strengthens the gastrocnemius and soleus muscles, which are the primary drivers of the calf pump mechanism. Starting with 10 to 15 repetitions and progressing over time is the standard approach.
Bicycle Pedaling (Supine): Lying flat on the back with hands at the sides, the patient lifts both legs and performs a pedaling motion. This promotes venous return through rhythmic muscle contraction and is particularly useful for patients who find standing exercises painful initially.
Leg Raises: From a lying position, one leg is lifted slowly off the floor, held for a few seconds, and then lowered gently. Alternating between legs encourages circulation without excessive strain on the valves.
Lunges: A step forward into a lunge creates a 90-degree bend at the knee, which tones the leg muscles and supports healthy venous return. This exercise can be introduced once the patient has progressed through initial ankle and calf exercises.
Buerger’s Exercises: This specific physiotherapy technique involves positioning the legs alternately in elevation and dependency to stimulate collateral circulation. The leg is raised above heart level to drain the veins, then lowered to allow refilling. This gravitational cycling improves blood flow dynamics in patients with chronic venous insufficiency.
Walking: Simple, consistent walking remains one of the most effective interventions available. A 30-minute daily walk activates the calf pump, improves venous hemodynamics, and requires no equipment. A walking program is specifically endorsed as a first-line exercise recommendation in clinical literature on CVI management.
2. Compression Therapy
Compression therapy is widely regarded as the gold standard conservative treatment for varicose veins. Physiotherapists are involved in fitting compression garments, educating patients on how to wear them correctly, and monitoring compliance.
Graduated compression stockings exert the greatest pressure at the ankle, which gradually decreases up the leg. This pressure gradient encourages blood to move upward and prevents pooling. The recommended compression graduation for most patients is 20 to 30 mmHg, which can be increased to 30 to 40 mmHg in more severe cases of chronic venous insufficiency.
The primary challenge with compression stockings is compliance, particularly in hot and humid climates like Bangalore’s. Physiotherapists address this through patient education on application techniques and by helping patients integrate compression wear into their daily routine.
Intermittent Pneumatic Compression (IPC) is an advanced form of compression therapy where a motorized sleeve is placed around the leg and inflates and deflates rhythmically to simulate the calf pump action. This is particularly useful for patients who are unable to exercise due to severe pain or immobility.
3. Complete Decongestive Therapy (CDT)
When varicose veins are complicated by significant edema or lymphedema, physiotherapists may employ Complete Decongestive Therapy. This multi-component approach combines manual lymphatic drainage, compression bandaging, specific exercises, and skin care to reduce swelling and prevent further fluid accumulation.
4. Kinesio Taping
Kinesio taping around the affected lower limb provides mild, continuous compression and proprioceptive feedback, which can reduce swelling and improve the patient’s awareness of limb position during daily activities. While not a standalone treatment, it serves as a useful adjunct to the core exercise program.
5. Hydrotherapy
Water-based exercises and contrast baths are often incorporated into physiotherapy programs for varicose veins. Contrast baths — alternating between warm and cold water immersion — stimulate blood vessel dilation and constriction, which can help relieve pain and improve circulation. Swimming is also an excellent low-impact activity that combines cardiovascular exercise with gentle compression from the water itself, making it well-suited for patients at various stages of the condition.
6. Electrotherapy Modalities
In clinical settings, physiotherapists may use electrotherapy tools such as Transcutaneous Electrical Nerve Stimulation (TENS) or Interferential Therapy (IFT) to manage pain and reduce edema, particularly in the early stages of rehabilitation when exercise tolerance is limited.
Lifestyle Modifications That Physiotherapy Addresses
Physiotherapy for varicose veins goes beyond exercise. A comprehensive program includes patient education on lifestyle factors that directly influence symptom progression:
Weight Management: Obesity increases intra-abdominal pressure, which impairs venous return from the legs. Even modest weight reduction can significantly ease symptoms. Physiotherapists often provide guidance on activity modifications that support healthy weight management without aggravating the veins.
Leg Elevation: Elevating the legs above the level of the heart for 15 to 20 minutes several times a day allows gravity to assist venous return, reducing swelling and discomfort. Patients are advised to sleep with the foot of the bed slightly elevated.
Postural and Movement Guidance: Patients are counseled to avoid prolonged standing or sitting. Setting a timer to move for a few minutes every 30 to 60 minutes is an effective strategy, particularly for desk workers. When sitting, keeping the feet elevated at or above hip height improves drainage.
Footwear Advice: High-heeled shoes restrict ankle movement and reduce calf pump activation. Physiotherapists recommend supportive, flat or low-heeled footwear that allows a full range of ankle motion during walking.
Dietary Considerations: While not a direct physiotherapy intervention, patients are educated on the importance of a diet rich in anti-inflammatory foods and adequate hydration to maintain healthy blood viscosity.
Post-Surgical Physiotherapy and Varicose Vein Recovery
When surgery is required – whether through vein stripping, endovenous laser ablation (EVLA), radiofrequency ablation (RFA), or sclerotherapy — physiotherapy plays a critical role in the recovery process.
Modern minimally invasive procedures such as EVLA and RFA offer high success rates, lower complication rates, and shorter recovery times compared to traditional open surgery. However, proper post-procedure rehabilitation is essential to optimize outcomes and prevent recurrence.
Immediate Post-Procedure Phase (Days 1 to 3)
Movement begins almost immediately after most varicose vein procedures. During the very first day, bed exercises — including rhythmic ankle movements and toe circles — are performed every hour to maintain circulation and reduce the risk of deep vein thrombosis (DVT). Compression stockings are applied as soon as possible and worn consistently throughout the waking hours, typically for a period of 3 days to 2 weeks as directed by the treating doctor.
Short walks of up to 10 minutes are encouraged from day 2 onward, increasing gradually in duration as comfort allows. Full weight-bearing on the affected leg is important – physiotherapists advise patients to minimize limping, as altered gait patterns delay recovery and can cause secondary musculoskeletal problems.
Early Recovery Phase (Week 1 to Week 2)
During this phase, low-impact aerobic exercise is the primary focus. Walking, gentle stretching, leg raises, and ankle pumps are all appropriate. Swimming can typically be introduced within the first week for procedures like sclerotherapy, though patients should confirm timing with their treating clinician.
Strenuous activities – including running, jumping, heavy lifting, and high-intensity resistance training- should generally be avoided for at least 14 days after the procedure. Activities that raise body temperature significantly, such as hot yoga, saunas, or prolonged hot showers, should also be avoided during this period, as heat promotes vascular dilation and may compromise the closure of the treated vein.
After sclerotherapy specifically, compression stockings and a 5 to 7 day restriction from vigorous exercise are standard recommendations.
Progressive Return to Full Activity (Week 2 Onwards)
Once the initial healing phase is complete, exercise intensity can be increased systematically. Walking sessions are extended progressively and can include inclines and longer distances. Resistance exercises targeting the calf and leg muscles are reintroduced, and patients are cleared for more demanding activities based on clinical assessment.
Throughout recovery, physiotherapists monitor for signs of complications, including increasing pain, swelling, warmth, or redness around the treated area, which may indicate infection or thrombosis and require prompt medical evaluation.
When to Seek Immediate Help After Treatment
Contact your physiotherapist or doctor right away if you experience:
- Sudden worsening of swelling or pain in the treated leg
- Redness, warmth, or hardness along the vein
- Fever or chills
- Unexplained shortness of breath or chest pain
These are rare but potentially serious signs that need prompt assessment.
Exercises to Avoid With Active Varicose Veins
Not all exercises are appropriate for varicose veins. High-impact activities that involve significant ground reaction forces or prolonged Valsalva maneuvers (breath-holding under strain) can increase intra-venous pressure and worsen symptoms.
Exercises to approach with caution or avoid unless cleared by a physiotherapist include:
- Heavy weightlifting with Valsalva breathing
- Long-distance running on hard surfaces without compression support
- Standing for extended periods without movement breaks
- High-impact aerobics or jumping exercises during active flare-ups
Swimming, cycling, yoga (restorative and non-inverted postures), and walking remain the most consistently recommended activities across clinical literature for patients managing active varicose veins.
How Home Physiotherapy Works for Varicose Veins in Bangalore
For patients managing varicose veins in Bangalore, traveling to a clinic multiple times a week can itself become a barrier to recovery — particularly when pain or swelling makes commuting uncomfortable. Home physiotherapy removes that barrier entirely.
At Physio at Your Doorstep, our registered physiotherapists visit your home across all major areas including JP Nagar, BTM Layout, Jayanagar, Koramangala, HSR Layout, and Whitefield. Each session is conducted on a one-to-one basis, allowing the physiotherapist to focus entirely on your assessment, treatment, and progress.
Our Orthopaedic Physiotherapy services cover musculoskeletal and vascular rehabilitation, including structured programs for varicose vein management. For patients recovering from vascular surgery, our Post Surgical Physiotherapy team designs phased recovery protocols to ensure safe, progressive return to normal activity. Older adults managing varicose veins as part of broader mobility concerns can also benefit from our Geriatric Physiotherapy program, which addresses the unique needs of aging limb health.
If you prefer to begin your consultation from the convenience of your home before scheduling in-person sessions, our Online Physiotherapy Consultation service is also available.
What to Expect From Your First Physiotherapy Session
If you are visiting a physiotherapist for varicose veins for the first time, here is what a typical assessment involves:
The physiotherapist begins with a detailed history, noting when symptoms started, which activities worsen or relieve them, any prior treatments, and relevant risk factors. A physical examination follows, which may include the Trendelenburg test (to assess saphenofemoral valve competence) and Schwartz test (to evaluate the saphenous vein system), alongside assessment of ankle joint range of motion and calf muscle strength.
Based on this assessment, a customized treatment protocol is established, which is then progressed at each session based on the patient’s response and tolerance. Clear goals are set — whether that means reducing swelling within 4 weeks, returning to pain-free walking within 6 weeks, or completing post-surgical rehabilitation milestones.
Resources and Further Reading
For those who want to explore the clinical evidence further, the following resources provide comprehensive information:
- Physiopedia: Varicose Veins Overview — clinical background, staging, and treatment options
- Shah R, Sadhu S. Role of Physiotherapy Interventions in Treating Varicose Veins. Medical Journal of Dr. D.Y. Patil Vidyapeeth. 2022;15(6):940-942
- PubMed: Physical therapy improves venous hemodynamics in cases of primary varicosity — randomized controlled study evidence
- PMC: Advancements in Varicose Vein Treatment — comprehensive review of modern treatment modalities
Take the First Step Toward Healthier Veins
Living with varicose veins does not mean accepting a life of discomfort, restricted activity, or permanent dependency on medication. Physiotherapy offers a clinically grounded, personalized approach to treatment that strengthens your legs, improves circulation, and supports lasting recovery — whether you are managing early-stage symptoms or rehabilitating after a vascular procedure.
If you are in Bangalore and looking for expert physiotherapy care that comes to you, book an appointment with Physio at Your Doorstep today. Our team of experienced, background-verified physiotherapists will assess your condition, design a treatment plan around your needs, and guide you step by step toward healthier legs — in the comfort of your own home.
Call us: +91 82337 87737
Email: physioatyourdoorstep24x7@gmail.com
This article is intended for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional for diagnosis and personalized treatment recommendations.